


April is our Birthday Fundraising Month – lets make it count.
Celebrating 32 years of awesome advocacy and the prevention of Meningitis Meningococcal Pneumococcal and related diseases in Australia.
Please support our ongoing work and host a Big Purple Breakfast party to raise funds. For an info pack, email: info@meningitis.org.au
Get your free signs and symptoms fridge magnet
Order NowI’d like to learn more about Meningitis
Signs &
Symptoms
Signs &
Symptoms
It’s important to know the warning signs and to get medical treatment fast!
Find out more
Vaccination & Prevention
Ways you can support us
Ways you can
support us
There are many ways you can support us; donate, volunteer, fundraise...
Find out more
Fundraising
I’d like to help!
Take part in community events or organise your own fundraiser to raise critical funds.


Survivor stories
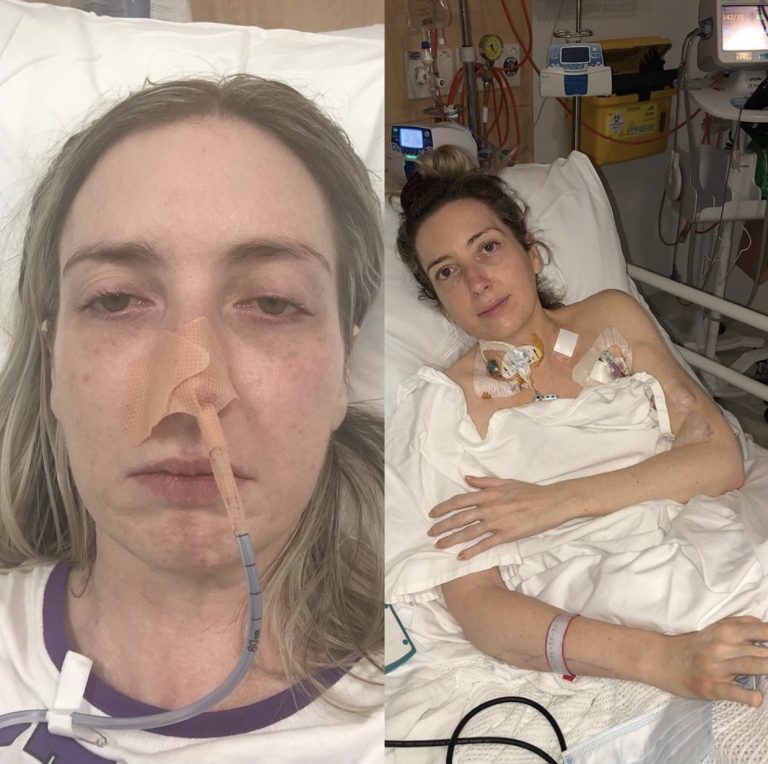
Sarah’s Journey to Hell
I went from being a happy independent working woman to fighting for my life within hours. I honestly thought I had a bad bout of the flu. Then, when my condition rapidly worsened, my mother took me to the hospital. It took meningococcal disease 12 hours to take hold of my body and shut it down.

Finn The Great!
It all began on the night of the 21st November 2013. Finn was just 13 months old. He was a happy little boy, but on this day he seemed to be sick with a cold. The only thing visibly wrong, was the shine above his lips caused from the constant runny nose he’d had. As the evening progressed so did his flu-like symptoms.

Kristen’s University Nightmare
My brush with Meningococcal Meningitis started on Anzac Day, 25 April 1998 at the age of 19 while I was studying at university and living at a college in Perth.
The symptoms began very early in the morning with a bad headache that crept into my bones making me extremely stiff and sore.
Previous slide
Next slide
